Case Report
1. You see a girl (Janet) of 14 years-old with her father in your office for a sore throat that you manage with success. Looking at this girl, you notice that she is obese and that no recent measurement of Body Mass Index (BMI) is included in her file. What should you do as a first step since the main issue at this time is her weight problem?
(a) you ignore the weight problem and discuss only the medical consequences associated with obesity.
(b) you measure her BMI.
(c) you arrange a follow-up with a dietitian for a weight loss program.
(d) you ask permission to discuss with the children and parents of the child’s weight problem and explore changes skills.
Answer: d
Explanations
(a) You ignore the weight problem and discuss only the medical consequences associated with obesity
HCPs can play an important role in the prevention and management of pediatric obesity, because they have long-term relations with obese children/adolescent and their parents. However, most primary HCPs feel ill-prepared to deal with this problem or even they perceive their efforts as inefficient [1]. They also noted obstacles to the proper management of pediatric obesity such as attitude and beliefs perceived by the children/adolescent and their parents, their own attitudes and beliefs concerning the problem of pediatric obesity as well as obstacles related to the clinical practice with this population (lack of time and motivation, inadequate medical equipment, etc.). Even considering these obstacles, ignoring the problem is certainly not the best approach, and it is contrary to what it is recommended in the prevention practice guidelines [2-4].
HCPs often associate obesity with their related medical consequences such as T2DM, HTN, dyslipidemia, CVD, orthopedic and other health problems. Those are certainly very good issues that need to be investigated. However, as a suggested approach since this patient is presenting without any other complaints, it is essential to determine the level of awareness of the children/adolescent and parents to the problem of the child’s weight and then to evaluate their ability to make one or more changes to improve or fix this problem. This process cannot be done without first asking for the permission to discuss the problem with the youth and her parents until you find other obesity-related problems. The best way to approach this patient and her father is by utilising the first A “Ask” of the “6As” model of counselling. For more information on the counselling approach of an obese patient the reader is refer to the “6As” model that is fully described in the article number 4, especially on the “ask” component of the model. The readers are also invited to read the most recent publications and books made by Dr Plourde on this counselling approach to have a complete explanation on the use of this counselling technique [5-8].
(b) You measure her BMI
The measurement of BMI is recommended as a practical measure for the prevention and management of pediatric obesity. It must be taken each year from the age of 2 years to follow the change of child’s weight status and its associated disorders. It can be taken at each visit of regular monitoring or when the patient presents for a specific health problem, as for our patient. The BMI measurement is the method most commonly accepted and used to track obesity in children and adolescent because it is a non-invasive measure. It is also a reliable indicator of body fat and correlates well with the complications associated with obesity [2-4]. Although it is recommended to perform the measurement of BMI in this young girl to evaluate her obesity and health risks, considering that this patient is obese, measuring her BMI is certainly relevant but first you should ask for the permission to discuss the weight problem and raise this issue with tact to avoid creating potential discomfort with the patient and her father. Overweight and obesity highly increase the risk of developing T2DM during childhood. There is also strong evidence that those who are obese during childhood are highly likely to be obese into adulthood and presents the obesity-associated complications [9].
(c) You arrange a follow-up with a dietitian for a weight loss program
This is certainly an approach that we should look after a discussion with the patient and her father and a more thorough assessment of her condition. Still, this shouldn’t be the first step. Weight loss is not generally recommended for children who are overweight as it may interfere with growth and development [5-8]. The main goal here is to keep Janet from gaining additional weight with hopes that she will grow into her current weight. With healthy eating habits and incorporating exercise, the emphasis should be on Janet’s new healthy lifestyle. Once she is finished growing, if weight loss is a concern, it can then be implemented. But, at this time, the priority is to ask her the permission to discuss her weight problem with her and her father. For more information on what should be included in this step of the counselling please refer to section “Arrange” component of the “6As” model of counselling.
(d) You ask permission to discuss with the children and parents of the child’s weight problem and explore changes skills
The first step and the most important in this case since you note that this patient is obese, is to ask the permission to discuss the problem of weight with the child and her father by asking the following questions or similar questions: “Are you concerned about your child’s weight and the effects of her weight on her health or quality of life? ‘’ Then you suggest the following statement: “Can we have a discussion about the problem of your child’s weight.” These questions can be modified to be adapted to the age and condition of the child [5-8].
The weight problem of a child is a sensitive issue that could embarrass the child and the parents. Therefore, you should proceed without issuing judgment. It is important not to blame or cause feelings of guilt among them. We must limit the medical jargon and use a sensitive and respectful approach. These discussions may provide to family physicians, pediatricians and other HCPs, as well as parents, better identification of personal or family environment factors which act as barriers to change. Talking about the advantages and disadvantages of modifications to the current behaviors can also help parents to reconsider what they can do to help their child [5-8].
2. During the discussion you learned that the patient has non voluntary loss few kg during the past 5 weeks and had more urination than usual during the past 4 days. There was no history of polyphagia, polydipsia or dysuria. But she mentioned that she feels more tired recently that she attributed to her recent episode of sickness including sore throat, cough and some fever. You learned that her mother had gestational diabetes while she was pregnant with Janet. She is now known T2DM since 3 years ago and presently she is on OADs. Janet is the second of three children but her siblings are well. There is a positive family history of T2DM in mother, maternal grandmother, maternal grand aunt, paternal uncle and paternal grandmother. Findings on physical examination were those of an obese adolescent (BMI-32kg/m2) not dehydrated with no evidence of acanthosis nigricans. Systemic examination was essentially normal. The blood pressure was 124/82 which was essentially comparable on subsequent visit. The patient and his parents have a sedentary lifestyle with plenty of time spent in front of the television, playing video games and little or no regular physical activity. Their eating habits are also inadequate; they consume a lot of fatty foods and sugary drinks and junk food. There is also a poor intake of fruits and vegetables. Random blood sugar at presentation was 11.9 mmol/l (N= 3.9 – 5.5 mmol/l), and Urinalysis showed +1 of glucose and absent ketones. A provisional diagnosis of T2DM was made.
What should be the next most important step(s)?
(a) you explain that you will make a full assessment of the problem, including personal and family risk factors associated with her condition.
b) you give advice and information on diets, physical activity and other modes of treatment programs to help parents make an informed decision on the most appropriate method to manage the T2DM problem of their daughter.
(c) you enter into a mutual agreement on the management goals of the T2DM of their child.
(d) assist the child and parents to recognize factors that may resolve the obstacles in the management of the T2DM problem of the child.
(e) explain the necessary follow-up with you, family physician or pediatrician, or other HCPs, according to the needs.
Answer: a
Explanations
a) you explain that you will make a full assessment of the problem, including personal and family risk factors associated with her condition.
It is important to perform a complete history, a general physical examination and appropriate laboratory tests to exclude any complications associated with the adolescent condition to be consistent with the “assess” component of the “6As” model of counselling. The history of the development of the adolescent, including possible delays of growth and weight gain mode must also be evaluated. Psychosocial history of the adolescent looking for a history of depression, eating disorders and the quality of life is also useful because it may indicate the need for a consultation in psychology or psychiatry. The family history of T2DM and associated disorders, including a detailed history of risk factors and complications (see article number 2), must be an integral part of the medical history. The history is complemented by questioning past and present, use of drugs including drugs taken by the mother during pregnancy and lifestyle, physical activity, eating habits, sleep patterns, family dynamics and socio-economic and environmental stress. You complete your assessment by performing a physical examination followed by the laboratory tests recommended (see laboratory testing) and those relevant from the medical history and physical examination. For more information on what should be included in this step of the counselling please refer to the appropriate sections of article number 4.
b) you give advice and information on diets, physical activity and other modes of treatment programs to help parents make an informed decision on the most appropriate method to manage the T2DM problem of their daughter.
Pending the confirmation of the T2DM diagnosis by the full assessment (item a), the patient and parents were counseled and placed on dietary control with elimination of SSBs such as juices, soda, reduction of foods with high glycemic index (GI) such as table sugar, ice cream, white bread etc. and increased intake of food with low GI such as pasta, skim milk, sweet potatoes, as well as reducing portion of food and increasing exercise as explained in question 1c. For more information on what should be included in the “Advice” component of the “6As” model of counselling.
As for our patient, the mean age at diagnosis reported for T2DM in youth is 14 years, coinciding with the relative insulin-resistance occurring during puberty, which may precipitate glucose intolerance [10-13]. Although adolescents presenting with diabetes are normally assumed to have T1DM, this may no longer be the case, even if the patient presents in ketoacidosis requiring insulin treatment. In recent studies 5 to 25% of children with T2DM presented with ketoacidosis, and ketonuria was present in a further 33%. The majority of these children are obese, but the severity of the obesity may be mitigated by weight loss prior to presentation [10-13]. These factors may lead to the misclassification of adolescents with T2DM as T1DM, and possibly an under estimation of the current prevalence of this clinical problem. Other pertinent features in the differential diagnosis include a positive family history; the frequency of a first degree relative with T2DM has been reported as ranging from 74 to100%, and the presence of acanthosis nigricans has always been regarded as rare in childhood but when present is strongly associated with obesity and insulin resistance [10-13].
The HCP should pay particular attention to the following points while in presence of an T2DM pediatric patient: 1). both environmental and genetic factors contribute to the etiology of T2DM; 2). a family history of T2DM indicates an increased risk for the disease; 3). the most important preventive measure for an at-risk individual is a healthy lifestyle, including regular exercise, weight management, and a diet low in fats and concentrated sugars and high in fruits and vegetables; 4). small proportion of diabetes mellitus is due to highly penetrant autosomal dominant mutations that result in maturity-onset diabetes of the young (MODY), a form of diabetes mellitus that resembles T2DM and 5). the lifetime risk of T2DM in the general population is about 5%. If a person has a biological relative with T2DM, the risk is increased. When a parent has T2DM, the lifetime risk for offspring is 10-15%. Risk is increased to a lesser degree if only a second-degree relative, such as an aunt, uncle, or grandparent, is affected [10-13].
In general the following are the red flags: i) obesity (as well as body fat distribution, especially central or abdominal body fat adiposity), lack of exercise, and poor dietary habits are all associated with increased risk for T2DM; ii). prevalence of T2DM is higher in some racial and ethnic groups, including African Americans, Native Americans, Hispanic Americans, Asian Americans, and Pacific Islanders; 3). early signs of T2DM include increased thirst, frequent urination, sudden weight loss, blurred vision, and fatigue or irritability as a result of changes in blood sugar levels; 4) history of gestational DM and a high birth weight, and impaired glucose metabolism [10-13].
(c) you enter into a mutual agreement on the management goals of the T2DM of their child.
It is essential to establish the objectives of treatment with the child and the parents. Well family doctors, pediatricians and other HCPs are best placed to determine the best course of action with regard to treatment but it is the patient and his/her parents who must do the work. However, currently, it is difficult to come to a mutual agreement without performing the complete assessment of Janet’s medical condition (item a). In the “mutual agreement” step of the “6As” model of counselling, you should gently mention that the long-term safety is a priority with children and adolescents diagnosed with T2DM and that achieving good glycemic control safely and without delay is a priority for newly diagnosed T2DM individuals [11]. As Janet is young preventing/delaying the onset of diabetes complications through getting optimal glycemic control is particularly important. In adolescents, the onset of T2DM points to a lot of potential complications if the disease is not adequately controlled for long periods of time [14]. An HbA1c as near to normal (< 7%) while minimizing the risk of hypoglycemia is appropriate [12, 15]. There is no need to be aggressive in selecting the general treatment target since Janet seems to have an appropriate family support and she seems highly collaborative; we can consider stronger treatment target if we have strong social and family support, absence of co-morbidities and complications and recent diagnosis [11], but this cannot be decided at this time since the full assessment (item a) of her condition has not been completed. The glycemic target should always be individualised based on a number of factors [11]. The American Diabetes Association has put in place a very nice graphical representation of individual physiologic and patient-centered aspects (https://durobojh7gocg. cloudfront.net/content/diacare/38/1/140/F1.large.jpg) that one should incorporate in the selection of our treatment target that we can then negotiate with the patient [5-8]. For more information on what should be included in this “mutual agreement” component of the “6As” model of counselling. You, Janet and the parents agree on a weight loss of approximately one pound per week for the next few weeks with diet and physical activity has this can have beneficial effects on improving her glycemic control as well as her lipid levels. You also agree on HbA1c (< 7%) glycemic target, but you postpone the final discussion until you complete the full assessment (item a) of her condition to rule out other co-morbidities and complications that could impact the glucose target [11].
(d) assist the child and parents to recognize factors that may re¬solve the obstacles in the management of the T2DM problem of the child.
Family physicians, pediatricians and other HCP must assist the child and parents overcome their barriers to weight and T2DM management as “assist” is another important component of the “6As” model of counseling. Patients and parents should be directed to resources promoting proper management of weight and T2DM. Assist means educate, recommend and support the child and his parents in the performing of their duties. Again a full assessment (item a) should be performed first in order to have a clear clinical picture of the clinical context.
Another approach that you can combine to the “assist” step is working on correcting negative health behaviors. Once families are ready to make a change, you can choose a behavior that children and parents want to change and for which they feel they can achieve successfully. A useful strategy is to help parents change the family environment to break the habit of the child to eat in an unhealthy way or stay sedentary. Parents can implement changes in the family environment so that healthy foods are more easily available and accessible than the unhealthy food which become less accessible and even absent from their environment.
Parents can also make it harder to access sedentary activities by removing the TV in the kitchen or in the bedroom of the child, to get rid of the remote control and put video games in a closet. They can make physical activity more accessible by playing with the children, by going to the park with them. These small changes in the family environment prevent known and unhealthy behaviors and promote the acquisition of new healthier habits. It is important to deliver this message to parents, because even a small change in behavior can make a big difference in the energy ingested or expanded and this can significantly improve the condition of the child [5-8].
(e) explain the necessary follow-up with you, family physician or pediatrician, or other HCPs, according to the needs.
Monitoring is essential to ensure that the medical recommendations can be met more easily. Family doctors, pediatricians and other HCP may need to negotiate with the child and parents the frequency of follow-ups, which will vary according to the condition of the child and the possibilities of family organization. If follow-up with other HCP is recommended, the relevance of this monitoring should be clearly explained to the parents and their agreement must be obtained before it is organized [5-8]. You will have to “arrange” for Janet and her family to be referred for a specialized diabetes nurses who will provide dietary and physical activity advices as well as teaching on self-monitoring of blood-glucose (SMBG), if the diagnosis of T2DM is confirmed after the complete assessment has been performed (item a). As mentioned, a provisional diagnosis of T2DM was made and a series of blood test was requested. For more information on what should be included in the “arrange” component of the “6As” model of counseling.
3. Two weeks after you received the following results. The fasting plasma glucose (FPG) was 12.8 mmol/L (N= 3.9-5.5 mmol/L); HbA1c was 10.2% (4-6%); Ketone body was absent; Tests for insulin antibody and antiglutamic acid decarboxylase (anti-GAD) were negative Cortisol level was normal with a value of 230.6nmol/l (240-418nmol/l), cholesterol level was elevated at 6.9mmol/l (<5.0mmol/l). The electrolyte results were within normal ranges with Sodium 137mmol/ l (128–142mmol/l), Potassium −4.4mmol/l (3.4–4.8 mmol/l), Bicarbonate − 25mmol/l (24–30 mmol/l), Urea−3.3 mmol/l (2.4–6.0mmol/l) and creatinine −75mmol/l (60–120mmol/l); C-Peptide 1.2 mmol/l (0.2-1.0mmoll); ACR 0.88 mg/mmol (<3.5 mg/mmol); eGFR 118 ml/min (90-120 ml/min). The definitive diagnosis was T2DM
What should be the next most important step(s)?
(a) you give advice and information on treatment options to help parents make an informed decision on the most appropriate option to manage the problem of their daughter.
(b) you enter into a mutual agreement on the management goals.
(c) help the child and parents to recognize the factors that can help resolve obstacles to T2DM management.
(d) explain the necessary follow-up with a nurse specialised in the treatment of T2DM.
(e) All of the above.
Answer: e
Explanations
(a) you give advice and information on treatment options to help parents make an informed decision on the most appropriate option to manage the problem of their daughter.
In the first follow-up discussion with Janet and her family you should explain the results that she obtained from the blood work (the chemical profile). You explain that based on the results, and the signs and symptoms she presented that she has T2DM. Because of her negative antibodies to GAD [15] and C-Peptide level we can exclude/confirm that she is not having T1DM. When we explained the laboratory results and discuss the diagnosis, we must limit the medical jargon and use a sensitive and respectful approach. You should explain that controlling her blood glucose is a priority for Janet, that the onset of T2DM at an early age point to a risk of multiple medical complications if the disease is not controlled for long periods [14]. However, because of her high C peptide concentration, this implies a certain degree of insulin resistance.
There are four different tests that can be used to diagnose T2DM. The first is the HbA1C test that is greater than 6.5% though there are some question as to how accurate these tests are as HbA1C levels might vary depending upon race/ethnicity. The second test that can permit a diagnosis is a FPG of greater than or equal to 7.0mmol/L. The third is of the two-hour plasma glucose or fasting glucose test which is a diagnosis if greater than or equal to 11.1 mmol/L during an OGTT. The last possible way to diagnose diabetes is by the symptoms – classic symptoms of hyperglycemia or hyperglycemic crisis which is random plasma glucose of greater than or equal to 11.1mmol/L. The standards for pre-diabetes are figured through similar tests but the numbers vary – these numbers are considered “normal but high” [10-13] The reason why Janet’s physician requested an autoantibody test as well as a C-peptide test is to ensure that the T2DM diagnosis is not being confused with T1DM. In obese children, screening guidelines for both T1DM and T2DM are very similar. C-peptide level is based on blood sugar level and is a sign that the body is producing insulin. A low levels or no insulin C-peptide means that the pancreas is producing little or no insulin. Janet’s C-peptide is high at 1.2 mmol/L while her GAD was negative. This means that Janet does in fact have T2DM and it is not being confused with T1DM. Because C-peptide level is high, this shows that her pancreas is still trying to overcompensate for the cells’ inability to take in glucose for energy.
Janet has cholesterol level of 12.8 mmol/L as mentioned earlier. This is high and due to her body’s inability to use blood glucose for energy and possibly a result of her high fat and high sugar diet, as well as her BMI of 31.0 kg/m². Her HbA1c level is an indication specifically of diabetes which was at an elevated level of 10.2% which is a measure of poor long-term blood glucose control. There was also protein and glucose in Janet’s urine which indicate that the kidney’s filtration ability has been altered.
In T1DM, there is a lack of insulin production caused by destruction of β-cells. In T2DM, insulin is produced but the tissues are insulin resistant and the body therefore has an increased need for insulin. To combat this, the pancreas produces more insulin but after too long the pancreas loses the ability to produce insulin at all. This result in T2DM which includes two metabolic defects: first insulin resistance and then insulin deficiency. Insulin resistance in T2DM is caused by a β-cell-receptor defect in which insulin cannot get into the cells and be taken up for fuel and then insulin deficiency which results in fasting hyperglycemia [10-13].
A pediatric patient with T2DM should be tested several times a year for protein in the urine. This is a sign that there is T2DM-related kidney damage as the kidney is allowing protein to escape the body without being absorbed. An extremely high amount of protein may be a sign of kidney disease. Kidney malfunctions and diabetes are related as kidneys are one of the organs that respond to the body’s glucose intolerance. Long-term glucose intolerance can harm the kidney, resulting with protein in the urine [10-13].
i) Potential Option: Lifestyle alone:
Achieving good glycemic control safely and without delay is a priority for newly diagnosed pediatric T2DM individuals [15]. As Janet is young preventing or delaying the onset of T2DM complications through optimal glycemic control is particularly important. In adolescents, the onset of T2DM points to a list of potential complications if the disease is uncontrolled for long periods of time [15]. Lifestyle interventions still form an integral part on any T2DM treatment regimen [15]. They can be considered in isolation for individuals with the glucose target of HbA1c (< 7.5%; 58 mmol/mol) [11]. Since Janet has marked hyperglycemia and even a strict diet and physical activity regimen is unlikely to restore her glycemic control, but would be certainly appropriate to correct her dyslipidemia.
ii) Potential Option selected: Lifestyle + metformin.
Metformin: Decrease HbA1c efficacy: high; hypoglycemic risk: low; Weight effect: Neutral/Loss; Major side effects: GI, Lactic acidosis; Cost: Low.
Choice of pharmacotherapy should aim to preserve β-cell function and improve insulin sensitivity; at present, metformin is the only OAD approved for use in children and adolescents [12, 15]. However Janet is severely hyperglycemic and metformin therapy alongside lifestyle interventions is unlikely to lower her HbA1c to the target level. Metformin would be expected to lower HbA1c by 1-2% leaving Janet with uncontrolled hyperglycemia [15].
iii) Potential Option: Lifestyle + Insulin .
Insulin: Decrease HbA1c efficacy: highest; hypoglycemic risk: high; Weight effect: Gain; Major side effects: hypoglycemia; Cost: variable.
Insulin can be considered alongside LSI from the onset for the treatment of T2DM in children and adolescents [11-12, 15]. For adolescents presenting with an HbA1c > 8% (69 mmol/mol) or severe manifestations of insulin deficiency, insulin is the most effective way to achieve rapid metabolic control [12]. However, Janet is nervous about the perspective of having to inject herself every day and is worried about weight gain since she is already obese. You should explain the benefits of using insulin to lower the risk of diabetes-related complications, that once glycemic control is obtained, it would likely be possible to switch to oral OAD (metformin) in combination with LSI.
(b) you enter into a mutual agreement on the management goals.
Following this discussion, the HCP and Janet decided upon a basal bolus of insulin regimen. Insulin regimens should mimic physiological insulin as closely as possible while achieving optimal glycemic control. Pre-prandial insulin should be divided into 3-4 pre-meal boluses; when regular insulin is being used, the basal: pre-prandial split is typically 30%:70% of the total daily insulin requirements For rapid acting pre-meal bolus, the basal pre-prandial split is typically 50%:50%. This is because regular insulin also provides some basal effects (10-15). The HCP and Janet decided to use rapid acting insulin for pre-meal boluses as it may reduce post prandial hyperglycemia and nocturnal hyperglycemia. Rapid acting insulin can also be taken immediately after food in order to increase flexibility.
During this short medical interview, you noted that one of the primary objectives of the child weight management is to improve her quality of life because she feels uncomfortable to play with the children of her age due to her weight. Therefore, she feels a bit excluded from her group. You also learned that neither the adolescent nor the parents are active physically. However, they do not seem to be very motivated by regular physical activity, despite the fact that this intervention could improve the skills of this young girl for the game and, therefore, have a positive effect on her quality of life. You agree, as a first step, to work on the reduction of sedentary behaviours such a reducing to less than 2 hours per day the time at watching TV or playing video games and gradually adding regular physical activity to promote physical fitness of this girl. You agree also on the importance to replace sedentary activities by low to moderate physical activities that parents and children would go to the convenience store, grocery store or another location nearby, foot or bike to increase in stages, physical activity, rather than taking the car [16].
(c) help the child and parents to recognize the factors that can help resolve obstacles to T2DM management.
Involving the entire family is important and ensures that the principle of treatment and the importance of LSI are clearly understood in order to permit appropriate level of support and encouragement from the entire family [13]. Education of the family and friends on the importance of lifestyle choices is essential [15]. Although Janet’s mother has T2DM, therapy is individualized and it is important that Janet’s family understands her individualized needs. In a family with more than one child, parental and sibling education may help prevent further development of T2DM in this family. Throughout the process, it is important to work with parents to verbalize clear and accessible objectives and discuss the steps to follow to achieve them. It is necessary to encourage parents to engage in healthy behaviours with the child/ adolescent and to serve as role models for change, an approach that has proved to be a good predictor of the success of the children in the management of their weight [5-8]. In this approach, the parents who eat vegetables, drink water instead of soft drinks, restrict the size of the portions of meals or snacks and engaged in physical activities with their children are more likely to encourage healthy behaviours in their children, because children learn by examples [5-8].
(d) explain the necessary follow-up with a nurse specialised in the treatment of T2DM.
You explain to the patient that insulin caries a risk of hypoglycemia and that SMBG is an integral part of optimizing Janet’s regimen. You explain that early optimization of blood glucose level will allow her for a rapid transition to oral therapy. For that Janet is advised to aim for the following blood glucose levels [13]: Pre-meal 5-7.2 mmol/L (90-130 mg/dL); Peak postprandial 10 mmol/L (180 mg/dL). You explain to Janet that in order to help her achieve these goals that you will refer her to a nurse specialized in the treatment of T2DM to learn about SMBG. The nurse will educate Janet on how to adjust insulin in response to daily glucose measurements and how to recognize and respond to hypoglycemia.
You explain that insulin is most effective when used in conjunction with an appropriate diet and exercise regimen to increase insulin sensitivity. For Janet the LSI must be specifically tailored to facilitate appropriate weight loss. In addition, to the advice on SMBG and the importance of adhering to the diet and exercise regimen, the diabetes nurses discuss the involvement of Janet’s family in the management of her diabetes. Janet and her family should be educated on SMBG – it is important to teach both Janet and her parents because Janet is young and may need assistance until she gets used to the system. SMBG is recommended with individuals with T2DM because it has been found to be very effective in controlling blood glucose levels. Tests should be done frequently in the beginning until patterns emerge and should be continued to be monitored around meal times, before and after physical activity, and before and after sleep. If Janet becomes ill then she must test her blood glucose every 4 to 6 hours with the same glucose targets as above.
According to the American Association of Diabetes Educators, there are many steps to educating those with diabetes. The first step is healthy eating as mentioned above, followed by being physically active. The nurse should teach Janet and her family members different ways to incorporate physical exercise into their daily routine such as going on family walk, taking more family outings that gets the family out of the home that are inexpensive alternatives to watching television (hiking, swimming, etc.). The nurse should then teach Janet and her family about monitoring and taking her insulin. This would have to be under the supervision of her parents as Janet is just 14 years old. Monitoring would include how to use a SBGM, knowing when to check the numbers and the meanings, the target range, and how to record blood sugar levels. This information should also be kept in Janet’s food journal especially at school. Any medications prescribed by Janet’s HCP should also be included. The nurse should stress the importance to Janet and her parents how important it is to follow this regimen. The next step is problem solving which looks at situations in which Janet may struggle to stick to her new, healthy lifestyle. For example, if there are no options at school for lunch that allow Janet to stick to her new diet or when she goes out with friends. The next step is healthy coping which is about adjustment to this new lifestyle, and the final step is about reducing risk which involves impaired awareness of warning signs of hypoglycemia [17]. For a complete example on problem solving, please consult the Chapter 7 of the book from Dr Plourde [5].
4. Then Janet has returned for her 6 month follow-up and since her diagnosis of T2DM, several insulin adjustments have been made to control her blood glucose level. Janet explain that she is feeling well but finds embarrassing to inject every day especially at school and when she goes out with friends. In addition she has managed very well to lose weight with good adherence to diet and exercise and she no longer feels exclude from the group. She expresses a strong desire to switch to oral therapy. You see that Janet’s journal on her cell phone has been meticulously completed and she has not experienced any problem with postprandial hyperglycemia in the past 3 months. Janet wants to transition from insulin to metformin. Her FPG: 6.7 mmol/L (120 mg/dl); her HbA1c: 6.3% (45 mmol/mol); her BP:120/80 mmHg; and her BMI: 26.7 Kg/m2 as well as a normal lipid profile.
True or False: you explain that she is doing very well on insulin and because of that it is preferable that she stays on insulin.
Response: False
Explanation
Both the risk/benefit ratio and the wish of each individual should be considered when designing treatment regimens. Janet is metabolically stable and is maintaining her blood glucose levels below her glycemic target. She has demonstrated a clear ability to manage her condition. Transitioning from insulin to metformin is therefore a possibility and something that Janet wishes to pursue. The insulin dosage should be tapered gradually to avoid hypoglycemia while steadily introducing metformin [11]. Transition from insulin to metformin can easily be achieved by decreasing insulin dose by 10- 20% each time the metformin dose is increased [11]. You should begin with metformin 250 mg once a day for 3 to 4 days then increase to twice a day if tolerated. Continue to titrate the dose in this manner over 3 to 4 weeks until the maximum dose of 1000 mg twice a day is reached. Meticulous SMBG is integral throughout this process; if the blood glucose reach the impaired range at any time, the taper should be slowed [11].
In conclusion, 3 years have elapsed since Janet was first time diagnosed with T2DM. She managed her T2DM well using metformin plus appropriate eating and regular physical activity. As a consequence, she is much happier and has lost 10 kg. Her FPG: 6.4 mmol/L (115 mg/ dl); her HbA1c: 6.1% (43 mmol/mol); her BP: 116/74 mmHg; and her BMI: 24.6 Kg/m2. The HCP continues to stresses on the importance of LSI to prevent disease progression for her and other member of the family. Now Janet is mostly an adult and if she begins to fail on metformin, she can return on insulin but she will be authorized to get access to a greater variety of OADs to control her T2DM and with the research progress she will eventually be able with the development of pharmacogenetics and pharmacogenomics to get access to personalized treatment.
References
- Plourde G (2012) Managing pediatric obesity: barriers and potential solutions. Can Fam Physician 58: 503-505, e239-41. [crossref]
- Lau DC. Douketis JD, Morrison KM, et al. (2006) Canadian clinical practice guidelines on the management and prevention of obesity in adults and children. CMAJ 176 : S1-13.
- Plourde G (2006) Preventing and managing pediatric obesity. Recommendations for family physicians. Can Fam Physician 52: 322-328. [crossref]
- Plourde G (2014) Paediatric obesity: A guide on diagnosis, prevention and management.
- Plourde G (2014) Les Jeunes et l’Obésité: Diagnostics et Interventions. Les Presses de l’Université Laval, Editors.
- Plourde G (2013) Six As model of counseling in obesity. Can Fam Physician 59: 353. [crossref]
- Plourde G, Prud’homme D (2012) Managing obesity in adults in primary care. CMAJ 184: 1039-1044. [crossref]
- Sharma AM (2012) The 5A model for the management of obesity. CMAJ 184: 1603. [crossref]
- Plourde G (2002) Impact of obesity on glucose and lipid profiles in adolescents at different age groups in relation to adulthood. BMC Fam Pract 3: 18. [crossref]
- Panagiotopoulos C, Riddell MC and Sellers AC (2013) Canadian Diabetes Association Clinical Practice Guidelines Expert Committee. Type 2 Diabetes in Children and Adolescents.
- Inzucchi SE, Bergenstal RM, Buse JB, et al. (2012) Management of Hyperglycemia in Type 2 Diabetes: A Patient-Centered Approach Position Statement of the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care 35: 1364 -1379
- Flint A and Arslanian S (2011) Treatment of Type 2 Diabetes in youth. Diabetes Care. 2011; S2:S177-S183Plourde G, Marineau JM. Reducing Sedentary Behaviours in Obese Patients. If they won’t exercise more – try to make them sit less. Parkhurst Exchange.
- Rosenbloom AL, Silverstein JH, Amemiya S, Zeitler P, Klingensmith (2009) ISPAD Clinical Practice Consensus Guidelines 2009 Compendium. Type 2 diabetes in children and adolescents. Pediatric Diabetes 10: S17–32.
- Del Prato S, LaSalle J, Matthaei S, and Bailey CJ on behalf of the Global Partnership for Effective Diabetes Management (2010) Tailoring treatment to the individual in type 2 diabetes practical guidance from the Global Partnership for Effective Diabetes Management. Int J Clin Pract 64: 295–304.
- Bailey CJ, Aschner P, Del Prato S, LaSalle J, Ji L and Matthaei S on behalf of the Global Partnership for Effective Diabetes Management (2013) Individualized glycaemic targets and pharmacotherapy in type 2 diabetes. Diab & Vasc Dis Res 10: 397–40.
- Plourde G, and Marineau JM (2011) Reducing sedentary behaviours in obese patients: If they won’t exercise more – try to make them sit less. Parkhurst Exchange 63-71.
- Plourde G, Klein AV, Dent R (2014) Impaired awareness of hypoglycemia in a man with type 1 diabetes. CMAJ 186: 770-771. [crossref]
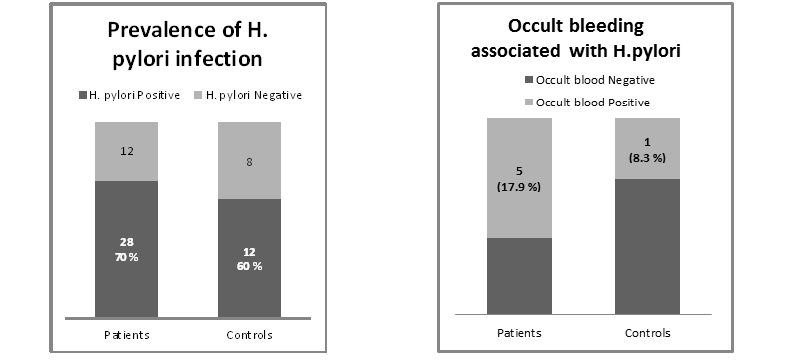
![Figure 1. Types of body fat mass distribution [15]](http://researchopenworld.com/wp-content/uploads/2017/01/IMROJ-2016-111-Fig1-1024x506.png)